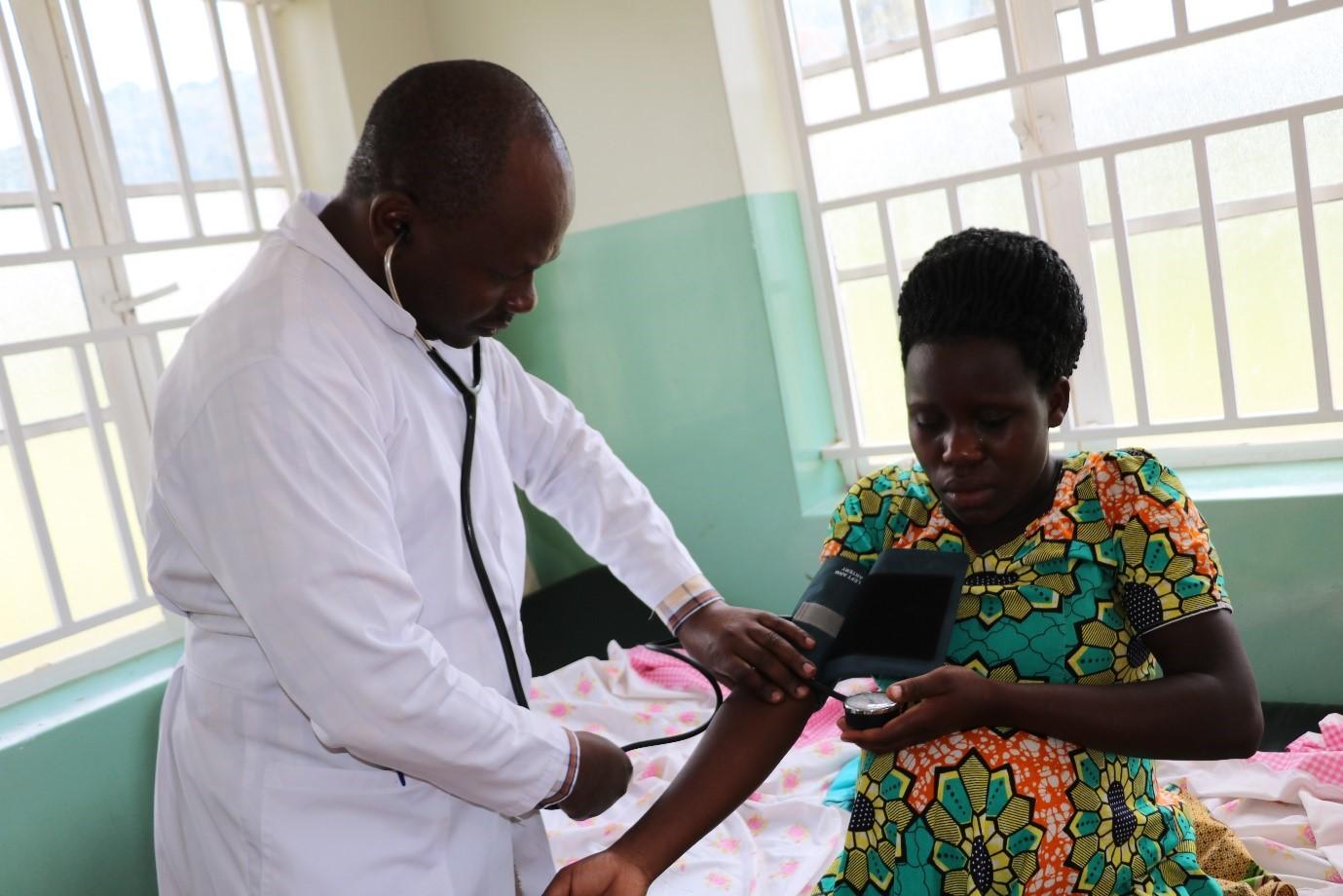
Quality low-cost health care services benefiting Uganda's Rwenzori and West Nile regions
52 years old Alfred Ocolla, has a
kidney and heart problem. He would travel 80kms away from his home to Arua
Regional Referral Hospital for routine check-ups. Sometimes, Ocolla would be referred
to Lacor hospital in Gulu for oxygen.
According to Dr Jammy Omara, the Medical
Superintendent of Nyapea hospital, the ultrasound department which was closest
to Ocolla was non-functional for 3 years due to lack of equipment. Hence, patients
including Omara who sought for ultrasound services were referred to Arua.
Today, several public health
facilities are faced with similar challenges including poor infrastructure,
human resource gaps and regular drug shortages.
Besides, the high cost of health
services especially at the private not-for-profit health facilities scared away many patients from seeking professional treatment thus resorting to
self-prescription, sharing of medicine and sometimes use of herbs.
To help change this situation, Enabel supplied the facility with a cardiography
and x-ray machine. Today, because of the new machines Ocolla receives his
routine check-ups at Holy Family Hospital, Nyapea located in his home area.
Since 2016, Enabel has been
implementing the National Results-Based Financing policy which provides for the
extension of direct financial support to health facilities to enable them purchase
equipment and other necessary items.
The funds are however provided on condition
that health facilities attain pre-determined targets. The organisation piloted this health
service delivery model in 80 health facilities including Holy Family Hospital
Nyapea.
Dr Sarah Byakika, the Commissioner
Planning, Financing and Policy at Uganda's Health Ministry, also the National Results-Based Financing
Coordinator, says the approach was adopted by government to improve
productivity and ensure access to quality health services for all.
“No doubt the delivery of quality health care services especially to
women and children in the two regions has improved,” Byakika said.
According to the In-charge Warr Health Centre IV in Zombo district,
Dr Imelda Kawambe, majority of the clients who seek services at the facility
are women with labour complications and children.
Flexibility in
utilisation of funds
Enabel's Project
Technical Officer Richard Musabe says the flexibility in utilisation of funds provided enabled beneficiary facilities to invest in critical
areas including infrastructure and incentivizing of front line
health workers.
“For our case, we recruited additional 2 clinical officers and
midwives but also enhanced staff salaries,” says Dr. Jammy Omara, the Medical
Superintendent of Nyapea.
For Maureen Kusemererwa, enrolled midwife Bundibugyo, the cash
incentives given to staff were an extra motivation.
“This motivated me to handle
mothers kindly especially during pregnancy, delivery and after,” she
said.
34-year old Harriet Kelike acknowledges the improvement in the
quality of care at Moyo general hospital, another facility benefiting from the
Results-based financing scheme.
The mother of 2 says the last time she delivered her child at the
facility, the baby was underweight. Kelike says the nurses closely monitored
and counseled her until the baby weight increased to 2.5kgs, “that is when I
was discharged,” the smiling Kelike says.
Increased deliveries at lower health
facilities
Another deliberate effort of the project was to reduce maternal and
child deaths by ensuring the quality of deliveries at HC III levels were done
under the care of a skilled health worker.
RBF support improved the quality of deliveries in the supported health
facilities. According to the District Health Information System (DHIS), deliveries at
the health centres increased to 64 percent compared to 49 percent at the start
of the project.
Reduced
congestion in general Hospitals
Investing in HC IIIs and IVs, Musabe says eased access to
services since patients nolonger have to travel long distances in search of
medication.
This he says reduced the number of patients admitted at General
Hospitals and HC IVs because lower-level health facilities are able to handle
most cases without referral to the higher level health facilities.
Better organised
referrals
Where referral is recommended, Dr. Byakika says prolonged delays
have been eliminated because of the now efficient ambulance system.
At Nyapea hospital for instance, the number of women coming for
antenatal services increased partly due to referral from lower level facilities.
The facility now carries out about 7 deliveries daily.
Reduced
user fees in private not-for-profit health facilities
According to Robert Nyakana,
Accountant Virika hospital in Rwenzori region, the reduced user fees led to an
increase in the number of people seeking medical attention.
“We used to get about 10 people per
day but today we get more than 25 patients a day,” Nyakana said.
Regina Kabasiita, a patient says the
hospital is now affordable to low-income earners.
Improved health
supplies
RBF focal person in Moyo, James Alule says previously medicine
would be prescribed before testing, against standard procedure, leading to inappropriate
drug use.
The facility was however revamped and various testing equipment
provided. Consequently, the number of patients increased from 80 to 450. The
facility has also registered 10% revenue increase.
Drug stock out was also tackled. Sr,
Juliet Asiimwe, Administrator, Rwibale HC IV says, this was the norm at the
facility, but then when the project started, the facility was given buffer
funds to stock essential drugs.
“Today, we get many clients coming here because
they are sure they will get the medicine available,” says Asiimwe.
Improved
data and financial management
Richard
Musabe says funds were also invested in financial training and book keeping
equipment to ensure up-to-date record keeping, proper data management and
accountability.
Dr Byakika confirms that the project was a stimulus for health facilities
to understand and analyse their data and timeliness in reporting which has
become a routine of keeping up-to-date data.
While the Results based financing approach has been a game-changer
in health service delivery, a lot still needs to be done to address poor
infrastructure, human resource gaps, inadequate medical equipment, frequent
drug shortages and low motivation of health workers if Uganda is to achieve universal
health coverage by 2030.
Latest news from this project
No news